Understanding Inflammation
Inflammation is one of the most misunderstood biological processes. It is typically portrayed negatively in popular media, yet inflammation is actually an essential protective mechanism. The challenge in discussing joint health and inflammation is maintaining accurate understanding of inflammation's complex, dual nature: necessary and protective when appropriately regulated, yet potentially harmful when dysregulated or chronic.
What is Inflammation?
Inflammation is a biological response to harmful stimuli—including injury, infection, irritation, or other stressors. The inflammatory response involves immune cells, blood vessels, and chemical mediators working together to contain and neutralize threats, remove damaged tissue, and initiate repair processes.
The classical signs of acute inflammation include redness, warmth, swelling, pain, and sometimes loss of function. These signs reflect underlying processes: blood flow increases (redness, warmth), fluid accumulates (swelling), chemical mediators stimulate pain receptors (pain), and the protective limiting of movement reduces further damage (loss of function).
The Inflammatory Process in Joints
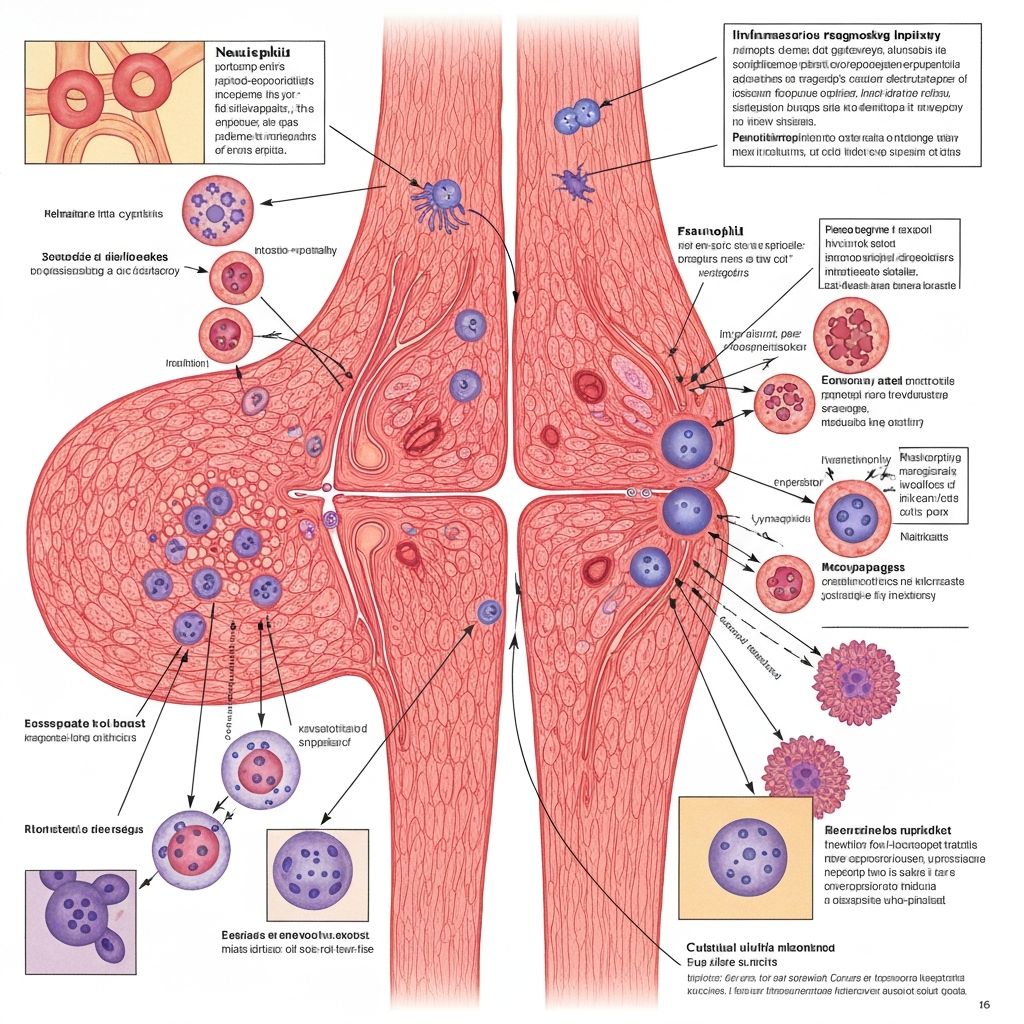
In joints, acute inflammation typically occurs in response to injury. When cartilage is damaged, ligaments are sprained, or other joint structures are injured, inflammatory cells rush to the area. These cells include neutrophils, macrophages, and lymphocytes. They secrete chemical mediators—cytokines, chemokines, prostaglandins, and others—that orchestrate the inflammatory response.
The acute inflammatory phase typically lasts from hours to days. During this time, the inflammatory response protects by preventing further injury (through pain and limiting movement), removes debris and damaged tissue through immune cell action, and initiates repair processes.
Acute vs. Chronic Inflammation
Acute Inflammation: A short-term, well-organized response to injury or infection. It's protective and necessary. Attempting to completely prevent acute inflammation after injury would actually be detrimental, as inflammation is essential for proper healing and tissue repair.
Chronic Inflammation: A prolonged, dysregulated inflammatory state that persists beyond the acute phase or develops in response to chronic stimulation. Chronic inflammation can be harmful, potentially contributing to tissue degradation and functional loss. Chronic joint inflammation is associated with various joint conditions.
The distinction is important: appropriate acute inflammation is protective, while chronic, dysregulated inflammation can be harmful. The goal is not to eliminate all inflammation, but to support the body's natural inflammatory regulation so that acute inflammation is appropriately initiated and resolved, and chronic inflammation is minimized.
Inflammatory Mediators
Cytokines: These are signaling molecules secreted by immune cells that coordinate inflammatory responses. Some promote inflammation (pro-inflammatory cytokines like TNF-α, IL-6, IL-1β) while others resolve inflammation (anti-inflammatory cytokines like IL-10).
Prostaglandins: Derived from arachidonic acid, these hormone-like molecules regulate various aspects of inflammation, including pain perception, blood flow, and the recruitment of immune cells.
Complement System: A cascade of proteins in blood that enhance immune responses by marking pathogens and damaged cells for destruction.
Other Mediators: Histamine, leukotrienes, bradykinin, and other molecules also participate in inflammatory regulation.
Resolution of Inflammation
A critical aspect of inflammation often overlooked in popular discussion is that inflammation is designed to resolve. The inflammatory process includes built-in resolution mechanisms. Anti-inflammatory cytokines are produced, prostaglandins that promote resolution are synthesized, and immune cells are signaled to stop the acute response.
Proper resolution is essential for healing. If inflammation fails to resolve appropriately, chronic inflammation can develop, potentially leading to ongoing tissue damage and functional loss. Supporting the body's natural inflammatory resolution processes is therefore important to joint health.
Factors Influencing Inflammatory Response
Physical Activity: Regular, appropriate exercise supports healthy inflammatory responses. Physical activity promotes the synthesis of anti-inflammatory factors and helps maintain the balance between pro- and anti-inflammatory processes.
Nutrition: Dietary components significantly influence inflammatory responses. Omega-3 fatty acids promote anti-inflammatory processes, while high intakes of refined carbohydrates and processed foods may promote chronic inflammation. Antioxidant-rich foods may help modulate oxidative stress associated with inflammation.
Obesity: Adipose (fat) tissue produces inflammatory mediators. Obesity is associated with elevated systemic inflammation, which can affect joints. Weight management therefore has implications for systemic inflammatory status.
Sleep and Stress: Inadequate sleep and chronic psychological stress both increase inflammatory markers and compromise the body's ability to regulate inflammation appropriately.
Natural Compounds: Various natural compounds have been studied for their effects on inflammatory processes. These include polyphenols from plants, curcumin from turmeric, ginger compounds, and others. While research is ongoing, some evidence suggests certain compounds may support healthy inflammatory responses.
Natural Compounds and Inflammatory Response
Many natural compounds have been traditionally used or are currently being researched for their effects on inflammatory processes. Understanding how these work requires distinguishing between:
Compounds that promote resolution: Some compounds may help support the natural resolution of inflammation, helping the body transition from acute inflammatory response to healing phase.
Compounds with antioxidant properties: Oxidative stress can amplify inflammatory responses. Compounds with antioxidant properties may help moderate oxidative stress and inflammatory responses.
Compounds affecting immune cell function: Some compounds may influence how immune cells are activated and function, potentially supporting more balanced inflammatory responses.
The Goal: Balanced Regulation
The goal in supporting joint health is not eliminating inflammation—that would be harmful and impossible. Instead, the goal is supporting the body's natural ability to regulate inflammatory responses appropriately: mounting appropriate acute inflammatory responses when needed, and properly resolving inflammation to prevent chronic dysregulation.
Conclusion
Inflammation is a complex biological process that is both necessary for health and potentially harmful when dysregulated. Understanding inflammation's dual nature is crucial to making informed decisions about joint health. Rather than seeking to eliminate inflammation entirely, the focus should be on supporting the body's natural inflammatory regulation through lifestyle factors (physical activity, nutrition, sleep, stress management) and understanding that well-designed natural compounds may support these regulatory processes. This balanced perspective reflects current scientific understanding of inflammation and joint health.